 This idea is further reinforced by studies that suggest that other herpesviruses, such as the Epstein Barr virus (EBV) and human herpesvirus-6 (HHV-6), may be related with multiple sclerosis (MS) and Alzheimer’s disease (AD), giving herpesviruses increased attention in the last decades on their potential roles in neurological diseases ( Casiraghi et al., 2012, 2015 Leibovitch et al., 2018). These observations have led to the notion that infection with HSV-1 may promote, or contribute to neurodegenerative disorders in humans ( Dobson et al., 2003 Otth et al., 2009 Martin et al., 2011 Buscarinu et al., 2017). On the other hand, because the immune system of an individual tends to decay upon aging, opportunities arise for HSV-1 to reactivate in the organism and spread to tissues such as the brain. The fact that HSV-1 is not invisible to the immune system and that immune cells are commonly found adjacent to infected cells, suggests scenarios in which immune cells infiltrating the CNS may somewhat contribute to chronic inflammatory processes that can be detrimental to the function of this tissue ( White et al., 2012 Van Velzen et al., 2013 Ma et al., 2014). This notion is supported by the fact that some studies have reported the presence of HSV-1 DNA in up to 65%–75% of the brains of seropositive individuals, without clinical signs of active infection or neurological illnesses ( Baringer and Pisani, 1994 Mori, 2010). Regardless if the individual is symptomatic or asymptomatic after infection with HSV-1, the lifelong presence of this virus in the organism may produce in some hosts alterations in cellular processes that are required for normal neuronal cell function, which could eventually lead to pathology in the brain in a fraction of seropositive persons ( Zambrano et al., 2008 Martin et al., 2014b). Nevertheless, HSV-1-infected asymptomatic individuals are significant reservoirs for this virus and contribute to its transmission through shedding ( Miller and Danaher, 2008 Ramchandani et al., 2016). Worldwide, nearly 60% of the population has antibodies against this virus, however only 20%–40% of those that are infected develop symptoms ( Looker et al., 2015). The virus is usually acquired during childhood and produces lifelong infections due to its ability to infect and remain latent in neurons ( Kramer et al., 2003). HSV-1 is the most common cause of sporadic encephalitis in adults, as well as the leading cause of infectious blindness in developed countries due to herpetic keratitis ( Whitley and Roizman, 2001 Lairson et al., 2003). 
Importantly, HSV-1 is a neurotropic pathogen with a wide spectrum of clinical disorders ranging from harmless skin manifestations, such as oral and facial lesions to severe infection of the central nervous system (CNS). Herpes simplex virus type-1 (HSV-1) is an enveloped double-stranded DNA virus belonging to the Herpesviridae family, that has a genome of approximately 152 kbp encoding more than 80 different open reading frames (ORFs Boehmer and Nimonkar, 2003). Furthermore, we discuss the impact of HSV-1 infection on brain inflammation and its potential relationship with neurodegenerative diseases. We review potential cellular and molecular mechanisms leading to neurodegeneration, such as protein aggregation, dysregulation of autophagy, oxidative cell damage and apoptosis, among others. Here, we review and discuss acute and chronic infection of particular brain regions by HSV-1 and how this may affect neuron and cognitive functions in the host. Importantly, there is accumulating evidence that suggests that HSV-1 infection of the brain both, in symptomatic and asymptomatic individuals could lead to neuronal damage and eventually, neurodegenerative disorders. Although HSV-1 encephalitis can be treated with antivirals that limit virus replication, neurological sequelae are common and the virus will nevertheless remain for life in the neural tissue. Once in the central nervous system (CNS), the virus can either reside in a quiescent latent state in this tissue, or eventually actively lead to severe acute necrotizing encephalitis, which is characterized by exacerbated neuroinflammation and prolonged neuroimmune activation producing a life-threatening disease. 
Herpes simplex virus type 1 (HSV-1) is highly prevalent in humans and can reach the brain without evident clinical symptoms. 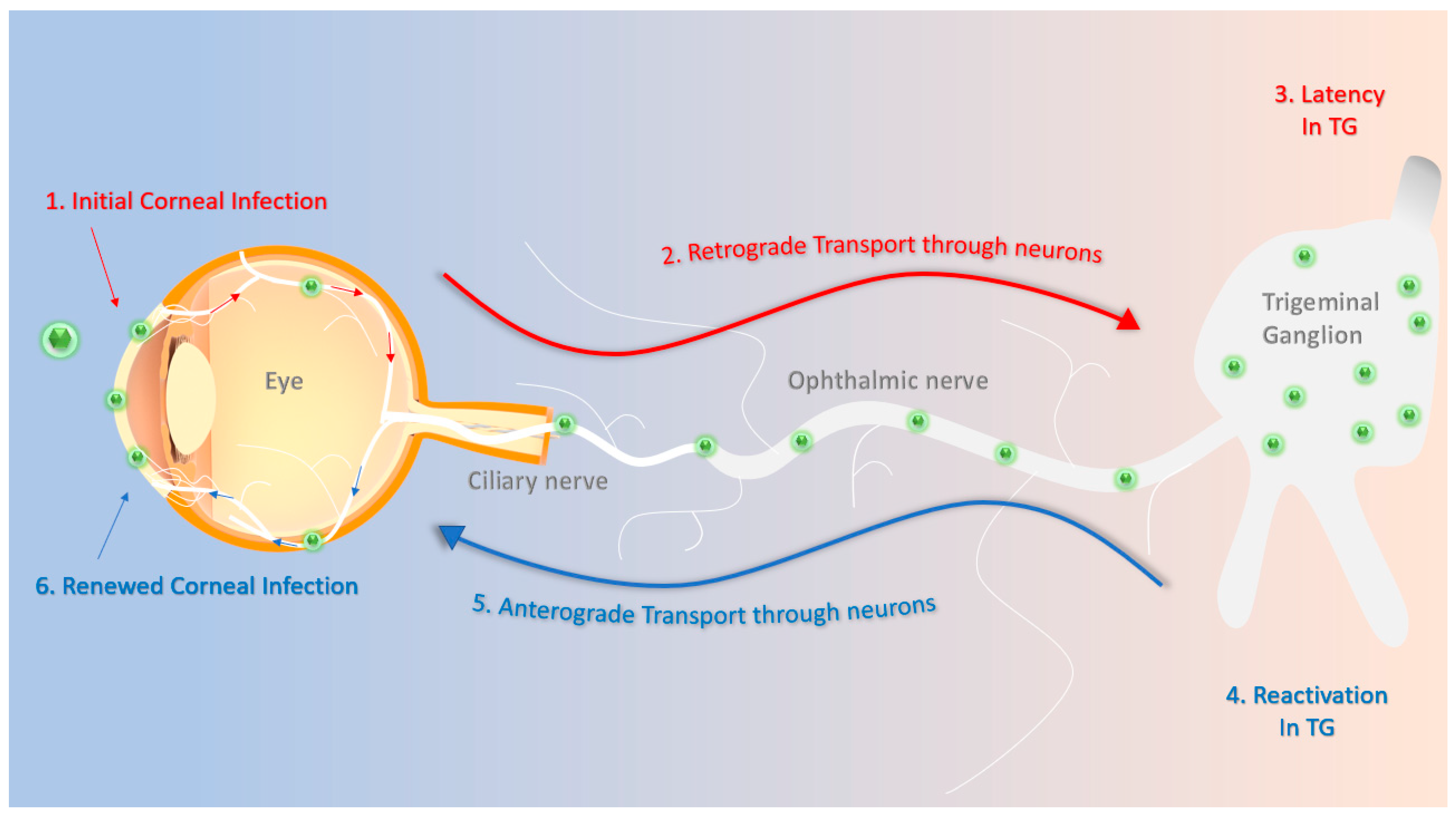
2Millennium Institute on Immunology and Immunotherapy, Departamento de Biología Celular, Facultad de Ciencias de la Vida, Universidad Andrés Bello, Santiago, Chile.1Millennium Institute on Immunology and Immunotherapy, Departamento de Genética Molecular y Microbiología, Facultad de Ciencias Biológicas, Pontificia Universidad Católica de Chile, Santiago, Chile. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
